Clinical Vignette
A 66 year-old male presents with recurrent syncope. 20 years ago, he suffered from ventricular fibrillation arrest following a brief episode of palpitations. An implantable cardioverter defibrillator (ICD) was inserted following a paroxysmal ventricular tachycardia (VT) and a sustained VT episode. Since then, supraventricular tachycardia (SVT), idiopathic VT and polymorphic VT were also detected by electrocardiography. In response, the patient was subsequently placed on long-term quinidine treatment to reduce the risk of developing VF episodes.
The ECG is:
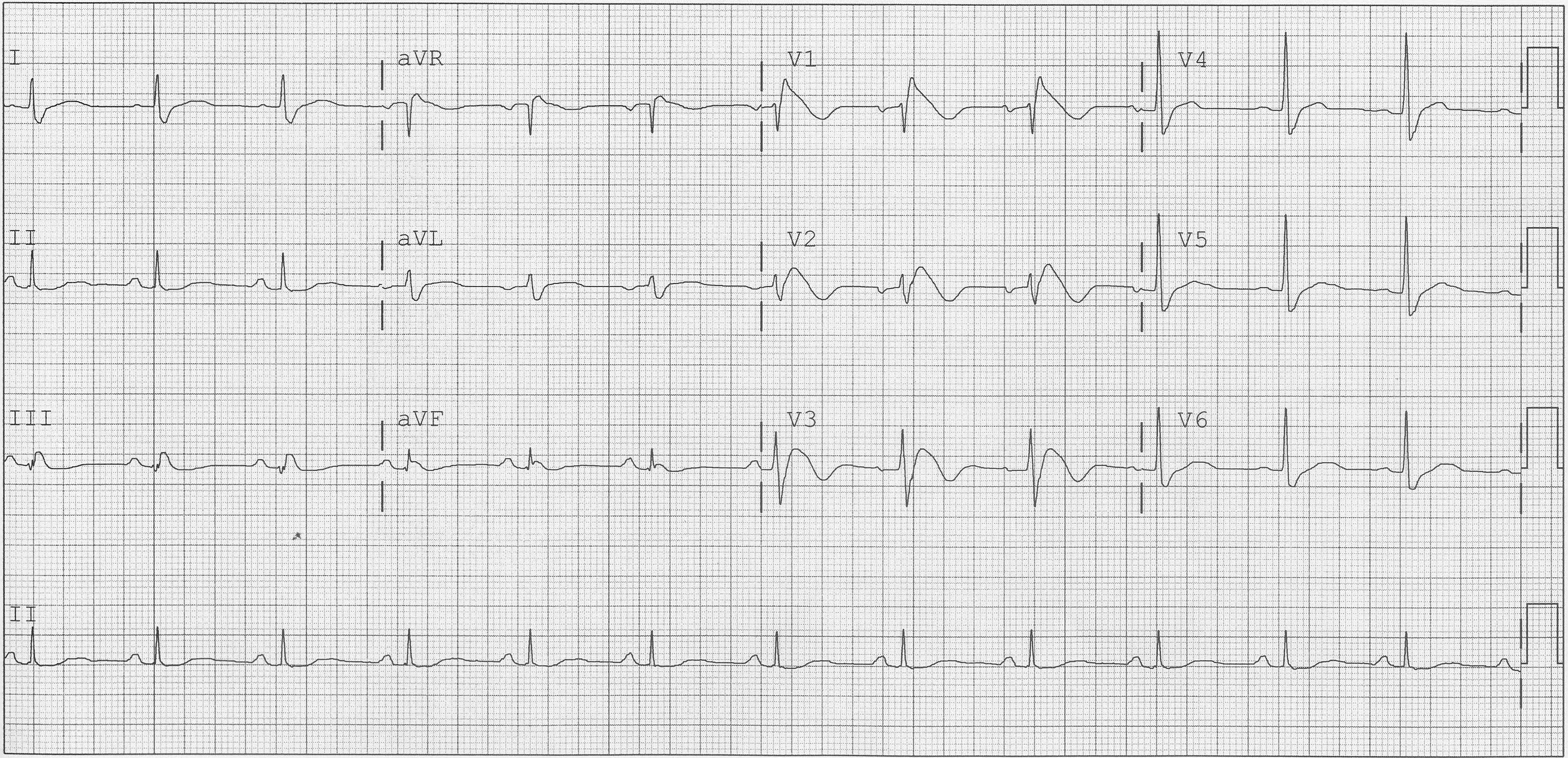
ECG Description and Analysis
1. Is it regular or irregular?
2. Is the heart rate normal, too fast, or too slow?
3. Can the main components of the ECG be seen? (P-wave before each QRS, QRS after each P-wave and a normal T-wave)
4. Are there abnormalities to the identified components in any lead? (Inverted T-waves, ST-elevation, terminal R’ waves, narrow/broad QRS complex, etc.)
The ECG is:

Let’s Analyze Case 4
At first glance, two abnormal features can be observed.
The QRS complex is prolonged at >120 ms accompanied by a RSR’ pattern in leads V1-3.
Also, a wide, slurred S wave in the lateral leads (I, aVL, V5-6) could be accurately identified.
These findings are suggestive of a RBBB pattern.
There are 3 main components in the ECG diagnostic criteria of RBBB:
• Broad QRS complex > 120 ms
• RSR’ pattern in V1-3
• Wide, slurred S wave in the lateral leads (I, aVL, V5-6)
Although RBBB may be benign, in many cases pathological causes involving the right ventricle can be identified.
These include right ventricular hypertrophy, cor pulmonale, and pulmonary embolism.
Other causes include rheumatic heart disease, cardiomyopathy, myocarditis, and atrial septal defect.
In this ECG, J-point elevation and/or a coved ST-segment elevation >2 mm in more than 1 of the V1-3 leads and negative T-waves are diagnostic of type 1 Brugada syndrome.
Exercise Based on Case 4
1. Use your calipers to determine the exact QRS duration.
2. Use your calipers to determine the J-point elevation distance from the isoelectric line.
3. Review all possible causes of RBBB and interpret it in the clinical context of the patient.
What’s Your Diagnosis?
Brugada Syndrome