Clinical Vignette
The importance of clinical and history and previous ECG tracings in the clinical interpretation of a patient with LAFB and syncope.
Male patient, aged 70yrs, recent history of unexplained syncope, intraventricular conduction delay on ECG at ER.
The ECG is:
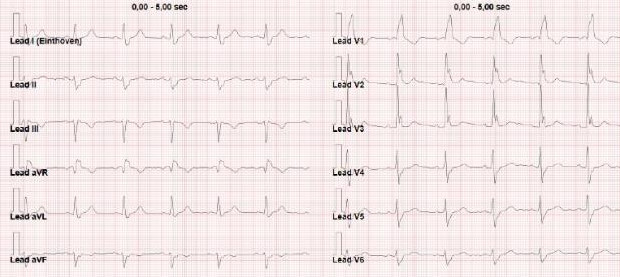
ECG Description and Analysis
In tracings with intraventricular conduction disturbances, three questions should be formulated:
1. What is the QRS axis?
2. What is the QRS duration?
3. What is the cycle length duration?
The ECG is:

Let’s Analyze Case 2
The ECG on admission (Figure 1) shows a bifascicular block, with left anterior fascicular block (LAFB) and right bundle branch block (RBBB) with QRS duration 160 msec and QRS axis -30°.
From the Hospital ECG data bank, it was possible to retrieve a previous tracing of this patient:
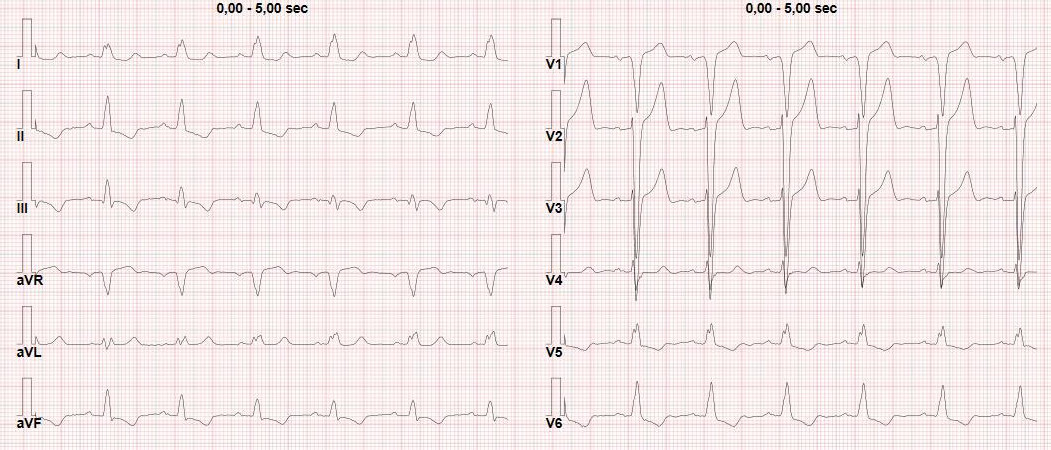
The previous ECG showed left bundle branch block (LBBB), with LAFB and left posterior fascicular block (LPFB), with QRS duration 140 msec and QRS axis 45° (at that time the patient was asymptomatic).
The comparison of the two tracings suggests a possible interpretation of this case:
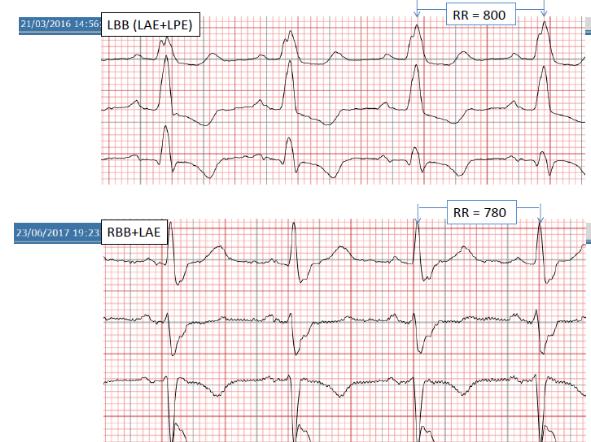
Upper tracing (2016): In presence of LBBB, i.e. complete block of both LAF and LPF, with a QRS duration of 140 msec, the activation of Purkinje fibers occurs by the RBB.
Lower tracing (2017): In presence of RBBB+LAFB, the activation of the Purkinje fibers occurs by the left posterior fascicular branch (LPF), with a QRS duration 160 msec.
As the RBB worsens its conduction, the impulse is only conducted along the LPF, already known to be delayed, therefore the syncope is probably due to a transient LPFB, giving rise to a trifascicular block.
Exercise Based on Case 2
1. Use your calipers to determine the QRS axis and QRS duration.
2. Review the criteria to define LAFB, LPFB, LBBB, and RBBB.
3. Review all possible causes of left and right fascicular blocks.
What’s Your Diagnosis?
The analysis of the two subsequent tracings, together with the clinical history of syncope, supports the hypothesis of a trifascicular conduction disturbance, which provides a strong indication for a pacemaker implant.